Revita Life Sciences
Hyperbaric Oxygen
Make Optimal Use of Oxygen: Oxygen the key to life
Hyperbaric oxygen therapy (HBOT) is a treatment in which patients breathe 100 percent oxygen while inside a hyperbaric chamber pressurized to greater than sea level (1 atmospheric absolute). For clinical efficacy, the pressures must be greater than or equal to 1.4 ATA. In clinical practice, pressures applied usually ranges from 2 to 3 ATA.
Treatment is delivered in multiplace chambers or in monoplace chambers, a single patient breathes compressed pure oxygen. In a multiplace chamber, multiple patients are exposed to pressurized air together while they each breathe pure oxygen through a face mask, hood or endotracheal tube. Depending on the indication, patients can be treated with up to 3 sessions of HBOT daily
PHYSIOLOGICAL BENEFITS
- Utilizing hyperbaric oxygen therapy can elevate inspired oxygen concentration by up to 1-1.5 times the normal levels. Consequently, arterial oxygen levels can surge up to 12 to 15 times the standard levels, resulting in a notable decrease in tissue hypoxia (hyperoxia, hyperoxemia).
- A tissue oxygen tension of 30mmHg is crucial for cell division and healing processes. Mitochondria, essential for oxidative phosphorylation and cytochrome c activity, necessitate a minimum tension of 5-3mm Hg.
- This therapy facilitates the mobilization, activation, homing, and differentiation potential of endogenous and peripheral stem cells, thereby serving as a valuable supplement in regenerative medicine.
- The heightened release of stem cells from the bone marrow leads to a substantial increase in CD34 cells and colony-forming cells (CFCs).
- Hyperbaric oxygen therapy also enhances the viability and proliferation of adipose-derived stem cells, modifies marker expression and subpopulations, and reduces TGF-β secretion.
- Additional benefits encompass fibroblast proliferation through fibroblast growth factor (FGF), promotion of capillary angiogenesis, reduction of edema, upregulation of vascular endothelial growth factor (VEGF), decreased nitric oxide (NO) levels resulting in vasoconstriction, as well as enhanced wound granulation and epithelial production.
-
- Vasoconstriction of arteries via VEGF to counteract edema.
- Stimulation of angiogenesis.
- Bactericidal activity.
- Enhanced extracellular matrix synthesis due to FGF, leading to increased collagen production.
INDICATIONS
WOUND HEALING
Hyperbaric oxygen therapy demonstrates significant benefits in various conditions characterized by delayed healing such as diabetic foot ulcers, gas gangrene, crush injuries, compartment syndrome, traumatic ischemia, osteomyelitis, radiation injuries, necrotizing soft tissue infections, compromised grafts and flaps, and acute thermal burn injuries. This therapy effectively promotes neovascularization and endothelial cell growth, enhances fibroblast proliferation, and facilitates collagen deposition, thereby accelerating the healing process in these challenging conditions.
NEUROLOGICAL
Hyperbaric oxygen therapy interrupts the detrimental cycle of cerebral ischemia, hypoxia, cerebral edema, and enzymatic disturbances. It preserves the integrity of the blood-brain barrier and enhances oxygenation of the cerebral ischemic penumbra, thereby restoring the arterial-perilymphatic oxygen concentration difference.
This therapeutic approach is beneficial for conditions such as cerebrovascular accidents, traumatic brain injury, cerebral palsy, Bell’s palsy, and idiopathic sudden sensorineural hearing loss.
LIVER DISEASES
Hyperbaric oxygen therapy (HBOT) has shown promise in alleviating liver oxidative injury, hepatocyte damage, bile duct proliferation, and fibrosis. Its antioxidant properties play a crucial role in reducing fibrosis and promoting liver regeneration. HBOT is particularly beneficial for liver regeneration in living donors post-liver transplantation and after hepatectomy. It enhances angiogenesis through increased VEGF levels in the regenerating liver and decreases MDA levels while increasing antioxidant activities such as GSH and SOD. Additionally, HBOT protects mitochondria during liver regeneration, as indicated by biochemical analysis of mitochondrial function.
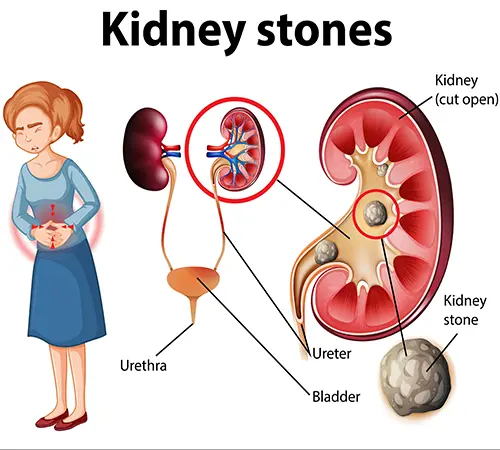
KIDNEY DISEASE
Hyperbaric oxygen therapy (HBOT) stands out as a valuable approach for tackling renal hypoxia in individuals grappling with Chronic Renal Failure. By elevating the partial pressure of dissolved oxygen, HBOT provides a targeted solution to improve renal oxygenation without imposing any undue changes to renal oxygen demand. Furthermore, this therapy exhibits a multifaceted impact by not only addressing hypoxia but also mobilizing tissue and peripheral progenitors. This mobilization fosters an environment conducive to their proliferation and contributes significantly to the repair processes essential for restoring renal function.
ANTI AGING
In today’s context, the idea of “normal” aging is under scrutiny due to widespread pollution in our air, food, and environment, alongside constant exposure to factors like automobile exhaust, second-hand smoke, and heavy metals. These environmental pollutants, combined with lifestyle choices such as alcohol, drugs, trauma, and infections, gradually erode the body’s resilience.
These insults lead to wounds throughout the body, notably observable in brain scans revealing areas of low blood flow and oxygenation, signaling decreased neurological function and premature aging, often leading to conditions like dementia.
Hyperbaric oxygen therapy (HBOT) emerges as a versatile solution for addressing these wounds induced by various insults. Regardless of their source, these wounds respond well to low-pressure HBOT treatments, making it effective in repairing chronic wounds associated with premature aging. This underscores HBOT’s potential as a universal treatment for wound repair, suggesting that individuals of all ages could benefit from its restorative effects.
DIABETES MELLITUS TYPE II
Hyperbaric oxygen therapy (HBOT) has been shown to ameliorate glucose tolerance and improve fasting blood glucose levels in diabetic patients. This effect may be attributed to the peripheral chemoreceptors known as carotid bodies (CBs), which respond to hypoxia by increasing minute ventilation and activating the sympathetic nervous system. In addition to their role in ventilation, CBs also regulate peripheral insulin sensitivity. Given that hyperoxia functionally blocks CB activity, HBOT could serve as a potential therapeutic intervention for type 2 diabetes by modulating CB function and improving insulin sensitivity.
CARDIO VASCULAR DISEASES
Hyperbaric oxygenation offers dramatic therapeutic potential in specific cardiovascular diseases associated with organ hypoxia, including:
- Coronary heart disease
- Cerebral vascular insufficiency
- Arterial insufficiency of the extremities
- Central retinal artery occlusion
- Surgical procedures requiring temporary interruption of circulation
Under hyperbaric hyperoxic conditions, oxygen is supplied to areas of the myocardium or other tissues with low oxygen tensions, allowing cells to maintain energy production and physiological function. HBOT provides short- and long-term synergistic benefits, offering relief from cardiac pain when used alongside medication. Its antiarrhythmic effects are attributed to increased parasympathetic activity and vagal tone, along with a suggested nitrogen-dependent beta-blockade of the heart. HBOT induces a reduction in cardiac output, stroke volume, and ventricular contractility, primarily through hyperoxic-induced bradycardia.